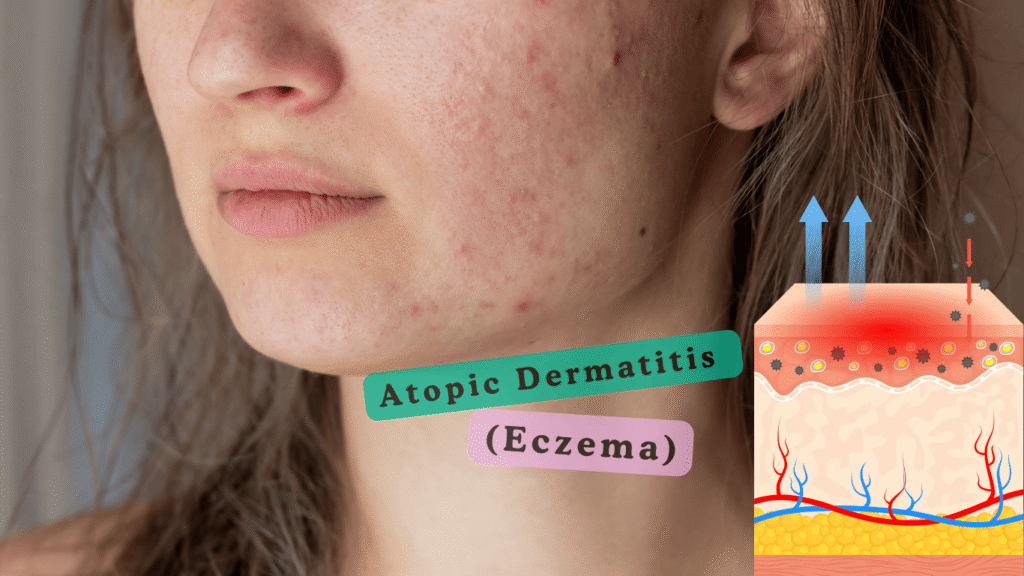
Atopic Dermatitis is a type of eczema It is not spread by touching any person commonly starts in childhood age, but it can also affect people of all ages it is long-term skin condition that causes dry, itchy, and inflamed skin. Which make our skin barrier weak and damaged skin barrier. Skin loses moisture easily and allows irritants, allergens, and bacteria to enter the skin. In response, the immune system treats these things as harmful and releases inflammatory chemicals against them, leading to Small red bumps that may ooze or crust, redness, swelling, and intense itching. This itching sometimes causes scratching, which further damages our skin and creates an ongoing itch–scratch cycle that worsens the condition. During flare-ups, triggers things like harsh products, weather changes, stress, or allergens can intensify this reaction, making the skin more inflamed, dry, and sensitive. treatment not getting on right time results repeated inflammation can thicken the skin and increase the risk of infection due to the weak skin barrier but it can be also make us uncomfortable and sometimes severe.
Atopic Dermatitis Causes
Atopic Dermatitis is caused by a combination internal and external factors factor such as genetic, immune, and environmental factors—not just one single reason. Where the skin barrier is become weak and unable to retain moisture properly. This makes the skin dry sensitive and gets irritated easily and quickly compared to normal skin. Also an overactive immune system reacts strongly to harmless substances like dust, pollen, or certain foods, leading to inflammation and itching. Environmental factors also play an important role. Avoid triggeres such as harsh soaps, detergents, weather changes, pollution, and allergens can more intense condition or cause flare-ups. In addition, stress and hormonal changes may further more serious symptoms by affecting the body’s immune response. atopic dermatitis is not caused by a single factor but by a mix of genetics, immune dysfunction, and environmental triggers, which together of these three lead to dry, itchy, and inflamed skin.
Genetic Factors (Heredity)
Genetics factor play a major role in the development of Atopic Dermatitis. If your family has a history of allergic conditions, your risk becomes higher.
Family History of Allergies: If parents or siblings have conditions like eczema, asthma, or hay fever, the chances of developing atopic dermatitis increase significantly.
Filaggrin Gene Mutation: A defect in the filaggrin (FLG) gene affects the skin’s ability to form a strong protective barrier. This makes the skin dry, weak, and more prone to irritation and allergens.
Weakened Skin Barrier (Inherited): Genetic traits can lead to a naturally thinner or less effective skin barrier, allowing moisture to escape and harmful substances to enter easily.
Higher Sensitivity to Irritants: People with inherited traits often have skin that reacts more quickly to soaps, detergents, dust, or chemicals.
Association with Atopic Conditions: Genetic factors are linked to the “atopic triad”-Eczema (Atopic Dermatitis), Asthma Allergic rhinitis (hay fever),
Early Onset in Childhood: Children with a genetic predisposition often develop symptoms at a very young age (infancy or early childhood).
Immune System Inheritance: Genes can influence how the immune system behaves, making it overreact to harmless substances.
Immune System Dysfunction
Immune system problems are a main cause of Atopic Dermatitis. In this condition, the immune system becomes overactive and reacts strongly to harmless substances.
Overactive Immune Response: The immune system mistakenly treats harmless substances (like dust, pollen, or certain foods) as dangerous, leading to inflammation in the skin.
Chronic Inflammation: Continuous immune activation causes long-term skin inflammation, resulting in redness, swelling, and irritation.
Imbalance in Immune Cells (Th2 Dominance): There is an imbalance in immune responses, especially an increase in Th2 (T-helper 2) cells, which promote allergic reactions.
Increased IgE Production: The body produces higher levels of Immunoglobulin E (IgE), an antibody linked to allergies, making the skin more sensitive.
Weak Defense Against Microbes: Due to immune imbalance, the skin becomes more vulnerable to infections from bacteria like Staphylococcus aureus.
Delayed Skin Healing: Immune dysfunction slows down the skin’s natural repair process, so irritation and damage take longer to heal.
Triggers Cause Strong Reactions: Small triggers like sweat, stress, or weather changes can lead to intense flare-ups because the immune system overreacts.
Auto-Inflammatory Cycle:
Itching → scratching → more inflammation → more itching. This cycle is driven by immune system activity and worsens the condition over time.
Skin Barrier Defect
A damaged or weak skin barrier is one of the main causes of Atopic Dermatitis. The skin barrier normally protects against moisture loss and harmful substances, but when it doesn’t function properly, problems start.
Loss of Moisture (Dry Skin):
A defective barrier allows water to escape from the skin, leading to dryness (xerosis), which is a common symptom of eczema.
Easy Entry of Irritants & Allergens:
Harmful substances like dust, pollution, soaps, and chemicals can easily penetrate the skin and trigger reactions.
Reduced Lipids in Skin:
The skin lacks essential fats (ceramides, cholesterol, fatty acids) needed to keep it smooth, strong, and hydrated.
Cracks and Micro-Damage:
Weak skin develops tiny cracks, making it easier for bacteria and allergens to enter.
Increased Sensitivity:
The skin becomes highly sensitive to environmental factors like heat, cold, and humidity changes.
Higher Risk of Infections:
A broken barrier allows bacteria (like Staphylococcus aureus) and viruses to infect the skin more easily.I
tchiness and Irritation:
Dry and damaged skin triggers itching, which leads to scratching and further damage to the barrier.
Poor Protection Function:
The skin fails to act as a proper shield, increasing inflammation and worsening eczema symptoms.
Linked with Genetic Factors:
Skin barrier defects are often connected to genetic issues (like filaggrin deficiency), making the condition long-term.
Symptoms of Atopic Dermatitis
Intense Itching (Pruritus):
The most dominant symptom. It can be severe and persistent, often worsening at night, leading to frequent scratching and discomfort.
Dry, Rough Skin (Xerosis):
The skin loses moisture easily, becoming dry, scaly, and rough due to a weakened skin barrier.
Redness & Inflammation (Erythema):
Affected areas appear red, irritated, and inflamed. In darker skin tones, it may look brown, purple, or gray instead of red.
Rashes (Eczematous Patches):
Irregular patches of irritated skin commonly appear on the face, neck, hands, inside elbows, and behind knees.
Swelling (Edema):
Inflamed areas may become swollen due to the body’s immune response.
Oozing & Crusting:
Small fluid-filled blisters can break open, leak fluid, and form yellowish or brown crusts, especially during flare-ups.
Skin Thickening (Lichenification):
Long-term scratching and rubbing cause the skin to become thick, hard, and leathery with more visible lines.
Cracked or Broken Skin (Fissures):
Severe dryness and repeated scratching can cause painful cracks, increasing the risk of infection.
Skin Discoloration:
The affected skin may become darker (hyperpigmentation) or lighter (hypopigmentation) over time.
Sensitive & Reactive Skin:
Skin becomes highly sensitive to irritants like soaps, detergents, perfumes, wool, and weather changes.
Burning or Stinging Sensation:
Some people feel a burning or stinging sensation, especially when applying products or during flare-ups.
Sleep Disturbance:
Constant itching and discomfort can interrupt sleep, leading to fatigue and reduced quality of life.
Recurrent Flare-Ups:
Symptoms tend to come and go, with periods of worsening (flares) triggered by allergens, stress, or environmental factors.
Treatment Methods for Atopic Dermatitis
Atopic Dermatitis is problem that continues for a long time Treatment is on controlling their symptoms, reducing the skin flare-ups, and repairing the skin barrier. Atopic Dermatitis treatment is take a long time to heal and restoring the natural defence system of our skin also preventing for future cure. This condition occur due to weak skin barrier and our overactive immune system response, by this our skin becomes dry, sensitive, and inflmmed. Best effective management strategy to controlling symptoms like small skin bumps itching, redness, and dryness, reducing the frequency and seriousness of our skin flare-ups, Repairing and strengthening the damaged skin barrier. Daily consistent skincare ( especially regular moisturizing) proper use of medications to calm the inflammation, and identifying and avoiding personal triggers such as allergens, irritants, weather changes, or stress.
Atopic Dermatitis also cannot be permanently cured, but it can be successfully managed with the right routine moisturizing and treatment plan.
Regular moisturizing

Moisturizing (Most Important Step)
Moisturizing s the most important step in managing Atopic Dermatitis because daily use helps repair the damaged skin barrier andreduce dryness and itching. Using rich creams or ointments with ingredients like ceramides, beta-hydroxy acid, glycerin, or petrolatum keeps the skin hydrated, reduces itching, and our skin get protects against irritants, allergens. It is best to apply moisturizer at least 2–3 times daily, especially immediately after shower or face wash when the skin is still little wet, to lock in moisture effectively.
Topical Corticosteroids
Topical corticosteroids are anti-inflammatory medicines applied directly to the skin to reduce redness, swelling, and itching. TCS are commonly prescribed treatments for conditions like Atopic dermatitis, contact dermatitis, and other inflammatory skin disorders. these Medications = clam down our immune response in the skin, which helps to control flare-ups for a quick relief from symptoms. they are available different strengths—light, average, intensive—depending on the seriousness of the condition and the area being treated. For example, mild steroids (like hydrocortisone) are frequently used on sensitive areas such as the face, while stronger used for thicker skin areas like the hands or feet. Use them exactly as prescribed because overuse or long-term use can do side effects such as skin thinning, stretch marks, or increased sensitivity.
Topical Calcineurin Inhibitors
Topical calcineurin inhibitors are steroid-free medications commonly used to treat the skin inflammatory problem like Atopic Dermatitis. They help to reduce the redness, itching, and swelling by suppressing the our immune response in the skin, by using them they do not cause skin thinning like but unlike corticosteroids. This makes them especially useful for especially in the areas such as the face, eyelids, neck, and skin folds.
Common examples include tacrolimus ointment and pimecrolimus cream. These are usually prescribed when topical corticosteroids are not suitable to the person, not effective enough, or need to be avoided for long-term use. TCIs can be used during flare-ups and also as maintenance therapy to prevent future flare-ups when applied a few times a week.
Some people may experience a mild burning or stinging sensation when they first apply these medications, but this usually improves with continued use. While they are considered safe when used as directed, it’s important to follow the medical advice and avoid excessive or unnecessary application. TCIs offer a good alternative for long-term management, especially in sensitive skin areas where steroid use is limited.
Antihistamines (For Itching Relief)
Antihistamines are medications commonly used to reduce itching (pruritus) skin conditions like Atopic Dermatitis and allergic reactions. They work by blocking histamine, a chemical released by the body during an allergic response that causes itching, redness, and irritation.
There are two main types of antihistamines: sedating (first-generation) and non-sedating (second-generation). Sedating antihistamines, such as diphenhydramine, can make you feel sleepy and are frequently helpful at night when itching interferes with sleep. Non-sedating options, like cetirizine or loratadine, are usually taken during the day as they cause less drowsiness.
While antihistamines can help relieve itching, they do not treat the underlying inflammation of eczema. That’s why they are usually used alongside other treatments like moisturizers and topical medications. It’s important to use them as directed, especially in children, and consult a healthcare provider for the right choice and dosage.
Atopic Dermatitis (Eczema)
What is the 3 minute rule for eczema?
The 3-minute rule for Eczema means applying moisturizer within 3 minutes after bathing to lock in moisture.
This helps keep skin hydrated, reduce itching, and prevent flare-ups.
How to clear eczema in 3 days?
You can’t completely clear Eczema in 3 days, but you can calm a flare-up quickly with the right care.
In 3 days: moisturize frequently, use prescribed creams (like mild steroids or non-steroid creams), avoid triggers, take lukewarm baths, and use antihistamines if needed—this can significantly reduce redness, itching, and irritation.
What causes Atopic Dermatitis?
It is caused by a combination of genetic factors, a weakened skin barrier, immune system overreaction, and environmental triggers like allergens, pollution, and weather changes.
What is the best moisturizer for eczema?
Thick, fragrance-free creams or ointments with ingredients like ceramides, glycerin, or petroleum jelly are best for maintaining skin hydration.
home remedies effective for eczema?
Home remedies like coconut oil, aloe vera, oatmeal baths, and cold compresses can help soothe symptoms but should be used alongside medical treatment.

Pingback: How To Treat Different Types Of Allergy On Face - Healixcare